I was in high-school when, for the first time, I bought my first emergency contraceptive pill. No, it wasn’t for a ‘biology project’, although that is exactly what I told the shopkeeper. Not because he asked, but because I felt the need to provide him with a reason—a socially ‘acceptable’ one. It was the first time my partner and I had something close to what conventionally heteronormative sexual intercourse is like. We both were novices and had very little idea about what all sex could mean. Courtesy? Our lousy sex and sexuality education in school that barely talked about sexual intercourse, contraception or sexual health and reproductive rights. We all could draw vaginas and penises for our exams and ‘tastefully’ call them, ‘female and male reproductive organs’ and giggle at every chance, without realising that these soon could become a part and parcel of our lives.
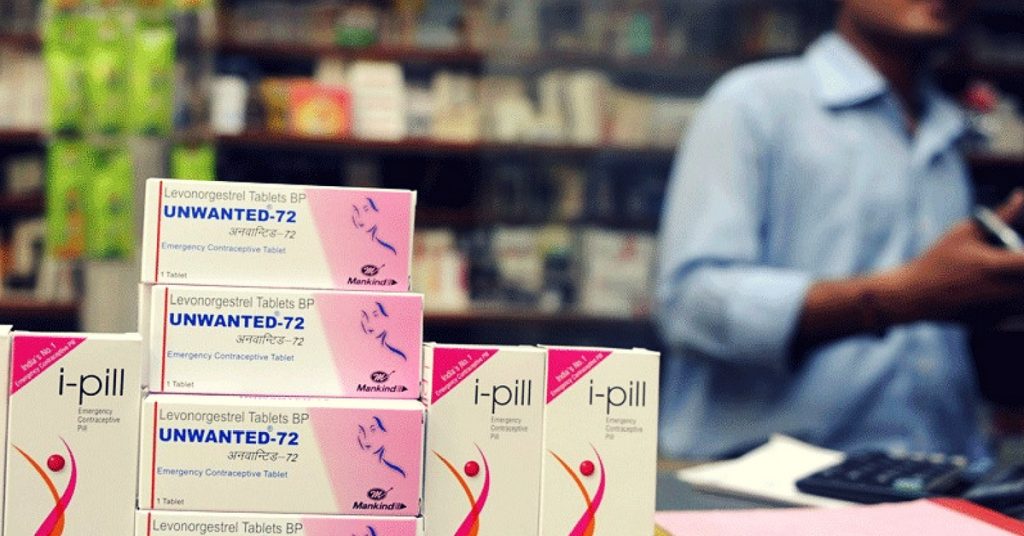
I did not have my periods after the first time we had sex and that meant only one thing—that I was pregnant at 16! Back in those days, the internet wasn’t much of a help, because I was intimidated by it and did not want to have a controversial search history. So I went and (wrongly) bought an iPill (influenced by TV commercials) after a month of the actual incident, and popped it as soon as I could. My partner, a teenager too, was anxious but couldn’t do much about the situation either. I still did not have my periods, and friends and their questionable sources of information suggested aspirins (a blood thinner, now banned without a prescription in India), various homemade recipes and hot baths to get my periods. But all I had was anxiety and occasional prayers to the ‘almighty’, promising them that I wouldn’t ever have sex again!
I did get my periods later and, I now realise, what my partner and I ‘did’ wasn’t enough to get me pregnant in the first place.
I, an urban, middle class privileged woman, with an English-medium school training and ample resources, had such health-threatening experiences and found very contentious information around contraception. Although the contraception in itself wasn’t inaccessible, due to my relative forms of freedoms, I still found myself in loose ends and went through a rollercoaster of emotions and risky decisions.
This made me think, what does accessibility to contraception even mean?
Is Accessibility to Contraception Solely a Matter of the Ability or Capability to ‘Buy’ a/any Contraception?
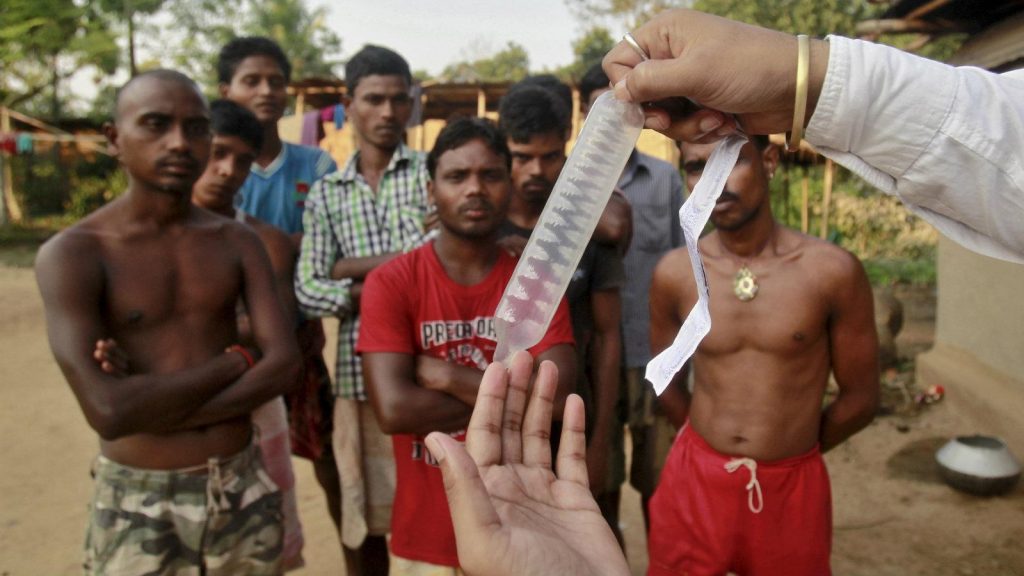
To a certain extent, and for a certain population, it is. The capacity to buy contraception is one of the most important factors that define accessibility. But the story does not end there. There are various brands that do provide the most commonly known contraceptive—condoms, at as low as 20 something rupees in India. The government of India too distributes free condoms through ASHA (accredited social health activist) workers at various government hospitals to promote birth-control and safe sex.
Accessibility isn’t solely restricted to buying or acquiring these common contraceptives or methods of contraception, but there are many indivisible factors that work around the issue of accessibility which determine what kind of contraceptives are available and accessed, who accesses them, who uses them and what knowledge around contraception is disseminated or, for that matter, even restricted by the society and its institutions.
However, reports show that the demand for free condoms have reduced over the years, due to the increasing number of options for contraceptives and their heightened marketing. Some experts also believe that myths around condoms too have had such impacts. Men often find it more ‘convenient’ for their women partners to simply pop an emergency contraceptive pill (which can be bought without a doctor’s prescription from most pharmacies) to avoid pregnancy, because they reckon that condoms ‘interfere’ with sexual intercourse and ‘compromise’ on sexual pleasure.

But are morning-after or emergency contraceptive pills safe for regular consumption?
In India, the most common motivation to use a contraception is often to avoid pregnancy. Other much more important factors like sexually transmitted diseases are either not an active rationale for using contraceptives or there is simply a dearth of knowledge about the various health consequences of STDs/STIs. Since premarital pregnancy is shamed and stigmatised upon by our patriarchal society, and even by gynaecologists, especially for the woman in question—as the ‘proof’ or ‘eye-witness’ of pregnancy is a part of her changing body—unwanted pregnancies then become a common reason to use contraception. Emergency contraceptive pills are only effective in preventing pregnancies (taken within 72 hours of having unprotected sex) but they do not act as safety nets for sexually transmitted infections.
Furthermore, research has repeatedly shown that the regular use of such pills have had health effects due to rapid hormonal imbalances in women’s bodies. However, these morning-after emergency pills have continued to be very popular in our country, making it the third largest market after the US and China, all together accounting for 73% of the global emergency contraceptive sales. Additionally, and on a more positive note, India has also seen a rise in the number of condom users, especially among the youth, thereby marking a shift from the regressive forms of contraception such as sterilisation to newer, more healthier options.
However, as recent as 2018, a study by the ministry of health and family welfare revealed that women still are the primary subjects of surgical birth control or sterilisation as per the Indian Family Planning Programme.
“Female sterilization remains the most popular modern contraceptive method. Among currently married women aged 15-49, 36% use female sterilization, followed by male condoms (6%) and pills (4%). Among sexually active unmarried women, female sterilization is the most commonly used method (19%), followed by male condoms (12%). More than eight in 10 (82%) women who got sterilized underwent the procedure in a public health sector facility, mostly a government or municipal hospital or a Community Health Centre (CHC) or a rural hospital,” the NFHS-4 reported.
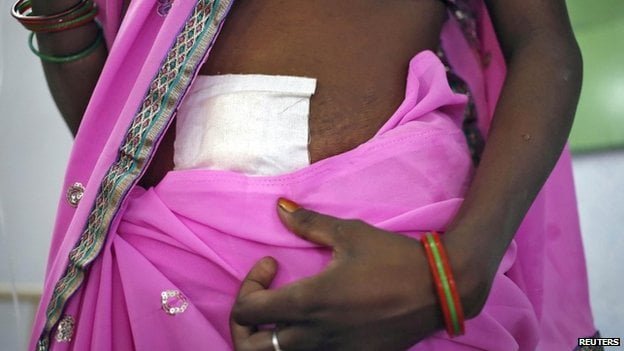
These sterilisation surgeries, often performed in deplorable medical conditions, have led to huge fatalities among women. Nevertheless, they still continue to be popular, especially among the marginalised groups because of monetary compensation as well as the influence of patriarchal mindsets that insist that women are primarily responsible for ‘planning their families.’ Various myths and misconceptions (like loss of virility/pleasure) around the male sterilisation surgery, which is a safer and simpler procedure, has also led to such a situation.
Hence, as depicted by the above cases in point, accessibility isn’t solely restricted to buying or acquiring these common contraceptives or methods of contraception, but there are many indivisible factors that work around the issue of accessibility which determine what kind of contraceptives are available and accessed, who accesses them, who uses them and what knowledge around contraception is disseminated or, for that matter, even restricted by the society and its institutions.
Accessing Contraceptives and Realising Intersectional Inequalities
It wouldn’t be very surprising if I told you that most of the women who are subjected to the oppressive, state-funded surgical methods of contraception come from rural-marginalised backgrounds and ‘voluntarily‘ register themselves into the sterilisation camps. These women, often belonging to lower castes, are forced to take up the responsibility of controlling the population of our country. This is not the result of recent policies, but are grounded within medical knowledge that was historically propagated by Western scholars and practitioners.
Marie Stopes, a ‘palaeobotanist and campaigner for eugenics and women’s rights,’ advocated birth control in India on claims that overpopulation and the consequent poverty was a result of ‘breeding’ by the ‘ignorant poor‘ and not because of the history of colonialism and its modern companions of capitalism and liberalism.
Such ideas, from the often over-glorified Western medicine stayed in the minds of the policy makers in India and led to flawed, regressive and even life-threatening family planning programmes that targeted the Indian poor. Their poverty overlapped with their identities as lower caste, rural, religious and gender minorities. Ironically, the health of the marginalised was compromised for the so-called ‘greater good’ of ‘a healthy nation-state.’ To reiterate, these methods of contraception again directed its focus on pregnancy aversion and remained ignorant towards the increasing risks of STDs/STIs.
Also read: The Sexual Politics In How Contraception Is Advertised
Knowledge around contraception was systematically curtailed by savarna eugenics which believed that the ‘unfit’—in this case the marginalised population—and their bodies should be made the testing grounds for contraceptives and these bodies must burden themselves with the responsibility of making a healthy nation, without being made adequately aware of the range of contraceptives available as healthier alternatives.
India did see more progressive anti-caste leaders like Sulochanabai Dongre, BR Ambedkar, and Periyar who not only advocated for the accessibility of modern contraceptives but also the need for education and sensitisation around its usage. Since Dalits were systematically excluded from public health resources and facilities, these leaders believed that contraception would not only result in ‘national good’ but also they would help in a holistic social upliftment of such economically backward marginalised groups in India.
Modern forms of contraception still remain limited to a few options, or their access and availability is catered for urban, educated, upper class/caste people, especially in developing countries like India. Rather, we could also argue that this very dearth of knowledge, both at the policy and individual levels, combined with systemic forms of discrimination, use such regressive methods of contraception, as per their convenience, disregarding the need for a better public health system for all. The state is barely afraid to leverage the bodies of women from various marginalised backgrounds, with promises of some mere monetary incentives.
However, India did see more progressive anti-caste leaders like Sulochanabai Dongre, BR Ambedkar, and Periyar who not only advocated for the accessibility of modern contraceptives but also the need for education and sensitisation around its usage. Since Dalits were systematically excluded from public health resources and facilities, these leaders believed that contraception would not only result in ‘national good’ but also they would help in a holistic social upliftment of such economically backward marginalised groups in India. They also emphasised on the liberation, autonomy and empowerment that contraception could bring for Indian women and their sexuality, as birth control is traditionally seen by patriarchal leaders as ‘sinful’, for they are believed to encourage sex before/outside marriage.
The Way Forward
As for me, the way forward from my 16-year-old self has been a comfortable one, as I was exposed to extensive, progressive and feminist literature around sex, sexuality and contraception. I would not lie—there were multiple pregnancy scares since then, but an approachable gynaecologist and a few dependable sources of information both outside and on the internet had helped me fight through the anxiety.
However, people from marginalised backgrounds do not share similar privileges and government organisations and educational institutions do very little for raising awareness among them. Sex and sexuality education, although made compulsory is hardly comprehensive even today, since our educators themselves have been internalising the shame around talking about sex in public spaces. There is a huge lack of sensitisation and the discomfort only gets reproduced over the years and across generations.
The marginalised often find themselves with imposed contraceptive methods. It is important to acknowledge that consent also pervades when it comes to contraception and must not only be understood only with respect to the ‘act’ of sex. Sex and sexuality encompasses the matters around contraception, and hence, forced or manipulated consent, such as in the case of sterilisation, is not only regressive but is very specifically an anti-minority stance. Such policies and their relevance need to be questioned and challenged.
Also read: We Need To Talk About Unsafe Sex And Our Dilemmas Around…
And to combat these on a more integrated sense, we need to follow the leadership established by our anti-caste leaders who believed in betterment, first and foremost, through an all-inclusive sex and sexuality education, thereby giving rise to well-informed policies which do not risk the bodies of the marginalised, but rather help them opt for more safer alternatives to prevent STDs/STIs as well as unwanted/unwarranted pregnancies.
This article is published as a part of the #MyBodyMyMethod awareness campaign on contraception. Feminism in India and Find My Method will be talking about the various forms of contraception, busting contraception myths and taboo and much more throughout the month of September, 2020. Find My Method works to provide accurate contraceptive information for a global audience. You can find localised information that is easy to understand, and is globally representative on Find My Method’s website and forum. You can follow them on Twitter, Facebook and Instagram.
About the author(s)
Pragya is a Master's Graduate in Sociology from Jawaharlal Nehru University. She works as the content editor at Feminism In India. She is also a ramen enthusiast, a hummus mother, a postcard hoarder and a wannabe cat lady. She still prefers writing on her notebooks, rather than on her laptop, but her job demands her to do just the opposite. Her favourite season is spring, and her alter ego is that of Mrs. Dalloway who said, "She would buy the flowers herself", in case no man ever buys her any!




