The 21st century has witnessed many changes in terms of travel and trade, urbanization, environmental degradation and other trends that increase the risk of disease outbreaks, their spread and amplification into epidemics and pandemics. At the same time, science and knowledge around infectious hazards are constantly evolving. However, the present novel Corona (SARS- COVID-19) pandemic has kind of put the entire world into a phase of partial lockdown even without letting science to deal with it in such a short period.
As the threat of COVID-19 has been increasing and the world has witnessed the exponential growth of Corona cases, alongside handling the crisis, it is also the need of the hour to revisit our health systems and preparedness to tackle such massive scale health crisis in the future. In general, public health systems are commonly defined as, “all public, private, and voluntary entities that contribute to the delivery of essential public health services within a jurisdiction.”
This concept ensures that all entities’ contributions to the health and well-being of the community or state are recognized in assessing the provision of public health services. However, this kind of system are mostly rendered as not being effective. The world’s advanced countries like Italy, the US and UK have such a form of the public health system. All of their health systems are failing completely to handle the COVID-19 crisis. However, the tiniest and poorest communist Cuba has been extending their help to countries in the world in order to tackle the crisis.
The Curious Case of Communist CUBA
The Cuban socialist revolution of 1959 not only gave birth to a socialist republic but a national healthcare system as well. The real transformation in the medical system did not come until about a decade post-Cuban Revolution. Cuba combines a completely Socialized Medical System that guarantees healthcare to all. This kind of healthcare system largely follows a proactive structural approach. The focus of this approach is providing preventative medical services, nationwide coverage and access to treatment. The preventative aspect of medical care has allowed Cuba to climb to the top of the world when it comes to vaccination and life expectancy.
Cuba combines a completely Socialized Medical System that guarantees healthcare to all. This kind of healthcare system largely follows a proactive structural approach. The focus of this approach is providing preventative medical services, nationwide coverage and access to treatment. The preventative aspect of medical care has allowed Cuba to climb to the top of the world when it comes to vaccination and life expectancy.
The unique healthcare system of Cuba is definitely far from perfect but it has presented a model for the world to follow. Cuba sent a group of doctors and nurses to Italy for the first time some days ago to help in the fight against COVID-19. This is the sixth medical aid team Cuba has dispatched recently abroad to combat the disease. Teams have been sent to Venezuela, Nicaragua, Jamaica, Suriname and Grenada.
It seems that this tiny Caribbean island nation is at the forefront of combating a global crisis now. With its cutting-edge innovations in preventative medicine and surgical technologies, Cuba is leading the world in healthcare, and we must look for ways to adopt such a health system in countries like India which is countries that still haven’t really invested in a universal healthcare system.
Health Care System in India
The constitution of India considers the “Right to Life” to be fundamental and obliges the government to ensure the “Right to Health” for all. Health is a state subject as per it. It is the responsibility of every state to make efforts for raising the health standard and the standard of living of the residents and the advancement of public health as its primary function.
The central government is responsible for international health treaties, medical education, and prevention of food adulteration, quality control in drug manufacturing, national disease control and family planning programs. It also sets national health policy including the regulatory framework and supports the states. India’s health system is based on the combination of public, private, and voluntary (both philanthropic and charity) entities. Despite being a fundamental Right, the public spending on healthcare has ensured that the country’s healthcare need has remained underserved and left for the private sector to service.
While North India is the most populated part of India, it has one of the most undeserved healthcare infrastructures in the country. Consequently, while hundreds of children died in hospitals in Uttar Pradesh last year, Kerala managed to contain the deadly Nipah virus outbreak within weeks, currently effectively tackling the COVID-19 crisis even much better than other Indian states. It was all possible in Kerala’s case due to its adequate investment in the health sector.
The fundamental aspect of a healthcare system is primary healthcare which is in shambles in India. There is only one primary healthcare center (often manned by one doctor) for more than 51,000 people in the country. The health care in India attracts huge investment with its result being contentious. It also stands among the cheapest health service provider in the world, yet highly unaffordable to crores of people who are most disadvantaged and vulnerable. A stark contrast in India’s health care system is, India has less than 1 doctor for 1000 patients (even lower than WHO’s the average target) but the medical tourism in the country is booming.
Healthcare is a state subject, the healthcare outcomes have remained divergent based on the quality of the state administration. While North India is the most populated part of India, it has one of the most undeserved healthcare infrastructures in the country. Consequently, while hundreds of children died in hospitals in Uttar Pradesh last year, Kerala managed to contain the deadly Nipah virus outbreak within weeks, currently effectively tackling the COVID-19 crisis even much better than other Indian states. It was all possible in Kerala’s case due to its adequate investment in the health sector.
Also read: Ecofeminism And COVID-19: Prejudices Of A Hindu Brahminical Society
How India is dealing with the current Health Crisis
Just a couple of days before the Janata Curfew was imposed, various universities across the country used numerous tactics to clear off campuses in the name of fighting the COVID-19 pandemic. The residents of various campuses such as Delhi University and its colleges, Jawaharlal Nehru University, University of Hyderabad, Maulana Azad National Urdu University (MANUU) and IIT-Bombay have abruptly cleared off their campuses.
Immediately after a positive case (apparently the information about patient’s death) was reported, the University has sent students home in such a way without even taking basic precautions like arranging for student transportation even when there was news on the spread of the virus in the community.
Some of these Universities may have retained their research scholars but most parts of these campuses are emptied putting students’ health in jeopardy by increasing the vulnerability to the pandemic. The Central University of Karnataka located in the Gulbarga district of Hyderabad-Karnataka region where the first COVID-19 death has been reported in the country went a step further. Immediately after a positive case (apparently the information about patient’s death) was reported, the University has sent students home in such a way without even taking basic precautions like arranging for student transportation even when there was news on the spread of the virus in the community. However, The UGC ultimately intervened too late (through an order dated 21 March), explicitly directing that university administrations cannot wash off their responsibility towards students, but campuses had already been emptied due to the vulnerability created by university authorities.
In what may come as one of the largest on-foot migration exoduses post-partition is took place for an entire week after the declaration of the lockdown. Migrant workers are made to travel on foot without the state providing them with any of the alternative travel arrangements. This happened when the government is ready to airlift its rich populace struck in foreign countries but stopped paying heed to the cries and sufferings of the workers who have greatly contributed to development of the nation. Those who have crossed the borders of Delhi and entered the peripheries of their states they met with most brutal forms of police treatment. In a most bizarre and inhuman incident at Bareilly in UP, they were made to sit and the Chlorine mixed with water has been sprayed on them.
Also read: Lock-Ups & Lock-Downs: Reflections On Indian Prison System During Covid-19
Looking at these disastrous ways of dealing with the crisis, I propose a country like India should adapt to a non-market public health system with food security and rationing at place disadvantaged groups and weaker sections.
References
- Sarah Farouq’s work titled ‘Cuba’s Healthcare System: A Political, Social, and Economic Revolution’ – Berkeley Political Review
- Five paradoxes of Indian Healthcare – The Economic Times
- Reimagining care and mental health- Hindustan Times
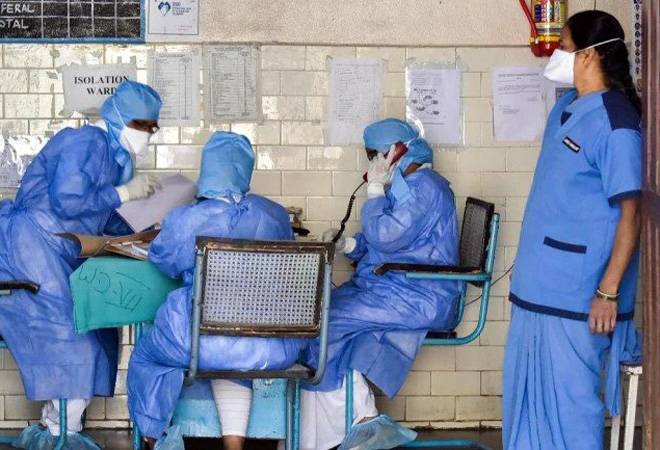
Featured Image Source: Business Today
About the author(s)
I am an education professional who has experience working in NGOs and schools involved in the task of improving school education and ensuring social equity in the academic sector, presently teaching as teacher educator in college. I am a graduate in social sciences, with an interest in teaching students at the secondary school level. My latest research interest is looking at the intersection of gender and caste in schools and on education overall.




lol typical left, you scratch my back, I scratch yours thinking.. Kerala is a disaster, currently topping the charts..
Wasn’t it too early to say that. Present scenario seems reversed and Kerala has contained virus smartly and wisely than anyone in this country.
Wasn’t it too early to say this Vijay? Present scenario seems reversed and Kerala has contained virus smartly and more effectively than anyone in the country. We must look at the no. of test done by states if you argue on the basis of no. of positive cases of covid-19.