Ovulation pain is the one-sided, pelvic or lower abdominal pain that some menstruators face, during the ovulation stage of their menstrual cycle. Ovulation refers to the menstrual cycle phase that involves the release of an egg or ovum, which occurs once every month. It usually occurs midway between the period cycle, with the exceptions of pregnancy or breastfeeding.
A minority of menstruators experience pain and discomfort during this stage. The duration and type of pain can vary, but it usually ranges from a few minutes to 48 hours, and can present as a mild twinge or severe discomfort. It can be hard to differentiate between ovulation pain and other types of pain, especially if people do not track their cycles, and are not aware of when ovulation occurs.
The exact cause of ovulation pain has not yet been determined. However, most researchers have settled on a few theories. As the egg develops in the ovary, it is surrounded by follicular fluid. When it matures, it ruptures from the follicle. This burst may cause some bleeding or release the follicular fluid that may irritate the lining of the abdominal cavity (the peritoneum), causing pain. Another theory hypothesises that during the development stage of the egg, the expanding follicle that gains maturity may stretch the membrane of the ovary, and trigger ovulation pain.
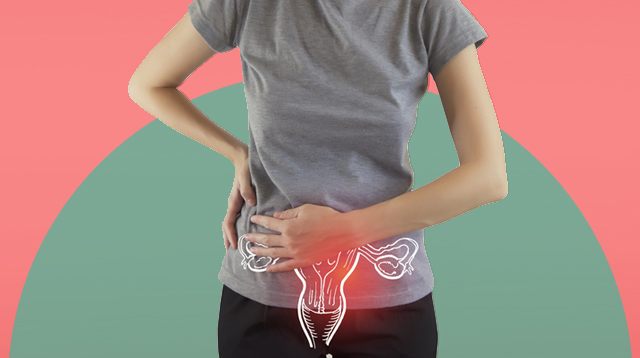
Symptoms of ovulation pain
The most prominent symptom associated with ovulation pain is pain in the lower abdomen and the inside of the hip bone. Pain can be felt on a specific side, depending on which ovary is releasing an egg. The pain may switch sides from the left to the right and vice versa, from one cycle to the next, or remain on one side for a few cycles.
There is a concerning lack of information and research on ovulation pain, especially since its exact cause is yet to be determined. A surprising lack of uniformity in information surrounding ovulation pain also persists, especially with regard to the statistics on the menstruators who experience it. This may be reflective of underreporting of such pain as well as a lack of awareness around ovulation pain
As per the person’s duration of the menstrual cycle, the pain can typically occur about two weeks before the period is due. Ovulation pain can vary across individuals, ranging from sensations such as twinges, sharp pains, cramps, or uncomfortable pressure. The pain can also last for varying lengths of time, from minutes to hours.
Light vaginal bleeding may also occur, accompanied by discharge. Nausea may also present itself, especially if the pain is severe. Due to the brief duration of the symptoms, there is no specific treatment for ovulation pain. Over-the-counter pain medication may be prescribed by a doctor according to the individual’s symptoms, to relieve the pain. Heating pads or warm water baths may also be helpful. Sometimes, estrogen-progesterone birth control pills may be prescribed to prevent ovulation pain.
Also read: What Is Vaginal Spotting?: Understanding Bleeding That Occurs Outside The Menstrual Cycle
The stigma and lack of concern surrounding menstruation leave a host of medical issues that are ignored or untreated. Pain, especially pain associated with menstruation is heavily normalised, and menstruators are taught to bear it in silence, and shamed for speaking about it. Dismal education surrounding menstruation, both in the education sector and in private homes leaves most menstruators ignorant of the mechanisms of the menstrual cycle, and any complications associated with it
It is important to diagnose the pain during the menstrual cycle, to receive treatment for the pain as well as rule out other underlying causes such as endometriosis or ovarian cysts. The doctor may diagnose ovulation pain based on the timing of the pain, and may also perform an abdominal and pelvic examination, which may include ultrasounds.
Moreover, to determine if ovulation pain is harmless, or a symptom of a more serious condition, doctors may require the patient’s medical history, as well as blood tests and cervical cultures. If the pain is severe, long, or associated with other symptoms such as fever, vomiting or redness, or burning at the site of the pain, it is important to immediately visit the doctor. Keeping a record of the menstrual cycle and the symptoms associated with different phases of the cycle is useful to identify and diagnose ovulation pain.
There is a concerning lack of information and research on ovulation pain, especially since its exact cause is yet to be determined. A surprising lack of uniformity in information surrounding ovulation pain also persists, especially with regard to the statistics on the menstruators who experience it. This may be reflective of underreporting of such pain as well as a lack of awareness around ovulation pain.
The stigma and lack of concern surrounding menstruation leave a host of medical issues that are ignored or untreated. Pain, especially pain associated with menstruation is heavily normalised, and menstruators are taught to bear it in silence, and shamed for speaking about it. Dismal education surrounding menstruation, both in the education sector and in private homes leaves most menstruators ignorant of the mechanisms of the menstrual cycle, and any complications associated with it.
This is troubling because not only do they continue to suffer pain without understanding the reasons behind it, but the dearth of knowledge around this also risks severe health complications, as well as possible unwanted pregnancies. It is crucial to build a greater consciousness about menstruation and any possible issues in association with it. The necessity of regular checkups, at least on an annual basis, with a gynaecologist should also be emphasised to ensure continued monitoring of menstrual health.
Moreover, menstruators should be taught the necessity of recording and tracking their menstrual cycle to ensure awareness of their body, identify possible risks, and seek help when needed. It is always important to pay attention to our own body so that we know when something changes and can address it at the earliest.
Also read: Vaginal Discharge And The Hidden Cost To Conform
Featured Illustration: Ritika Banerjee for Feminism In India
About the author(s)
Aradhana Choudhury is an aspiring policymaker. She is currently pursuing herMaster’s in International Development and is seeking to apply intersectional learningto development strategies. She has a keen interest in development research, policyanalysis, and gender. She hopes to support tangible impacts towards gender equalityand equity, with community participation at the forefront.Aradhana also has a keen interest in history and heritage studies and has worked toexpand the interest of general audiences in the history of a place




