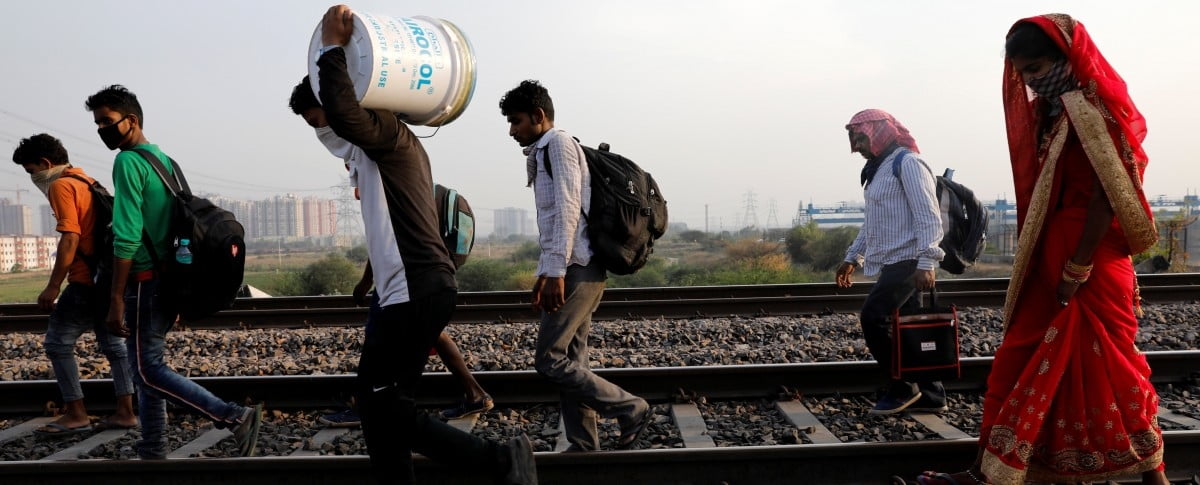The COVID-19 pandemic has brought conversations on mental health to the fore like never before. Given how we have suddenly lost companionship, people are finding it hard to open up to therapists on video, but many people, especially in India, simply even lack the means to do so. A pandemic of such great measure takes a toll on the minds of those belonging to discriminated communities, who are further pushed to the sidelines in such crises. It is important we, therefore, talk about the intersectional politics of wellbeing in a society as structurally diverse and hierarchical as ours.
An individual’s well-being cannot exist in a vacuum, it is tied to the systemic and structural bodies that we interact with, be it at the level of the government, policy, law, police, education, or economy. When we look at well-being from an individualistic perspective, or as something that an individual should strive for, we ignore the structural aspects of it.
An individual’s well-being cannot exist in a vacuum, it is tied to the systemic and structural bodies that we interact with, be it at the level of the government, policy, law, police, education, or economy. When we look at well-being from an individualistic perspective, or as something that an individual should strive for, we ignore the structural aspects of it.
Also read: Why Do We Need Culturally-Mindful Therapy?
Whenever a crisis such as COVID-19, for instance, occurs, it affects the minority communities the most and in every community, the most affected are the women, because women do not just have to face violence and discrimination based on their caste or religion but the oppression they face is multi-layered also because they are women. The mental health implications of crises that marginalised communities go through are extremely high and as we witnessed, especially increases in times such as the pandemic. So when someone said the pandemic is an equaliser, they were clearly in the wrong.
Migrant labourers had to walk back home with little or no food or relief from the government, Delhi pogroms of 2019-2020 saw Muslims getting killed. As news about how the Muslim residents were leaving their homes and moving away came to the fore and as they continue to be persecuted in our country, we can make an educated guess about the toll this must have taken on their mental health.
Surveys indicate that India has about 9000 psychiatrists for its 1.3 billion people and out of that only a few belong to the DBA communities. And so the question arises, how do we, and how many of us, understand the intersection of caste, religion, and mental health?
Right now in India, there are only a few organisations that help these communities that have been pushed to the sidelines. One such organisation is The Blue Dawn, which connects people from marginalised communities with affordable and accessible mental health services through an online portal. Yet, in India, today there is little to no representation of people from Bahujan communities at any level – media, cinema, or government – which is to say, there is a lack of policies that are affirmative towards communities marginalised by caste and other socio-political intersections, and of people from those communities in positions of leadership. How many women from DBA communities, transgender people, people with disabilities or queer individuals at these levels so often?
Also read: Why We Need An Intersectional Feminist Approach To Therapy
This has only gotten worse after the pandemic hit India. None of the migrant workers were given due diligence and had to walk home in the scorching heat with little to no food and water, those who took the trains were suffocated and killed because of lack of air and again the scorching heat, the police not only brutally beat them up but closed the borders leaving the migrants stranded. The repercussions of such levels of precarity must have not just been physical but mental as well.
The effect on the mental health of disadvantaged communities is disastrous and leads to non-pathological distress and mental health problems in minority communities. It also worsens pre-existing problems, for example, alcohol abuse, domestic violence, health problems, humanitarian aid related problems and anxiety due to financial problems, economic disparities, political subjugation, family separation, etc. This could also lead to increased violence against women and girls especially those that come from minority communities.
It is time we spoke about the effects caste discrimination, Islamophobia, homophobia and transphobia has on the mental health of the affected populations, coupled with the dread of the pandemic. It is also important to remember that these issues have already existed before COVID-19 before the pandemic.
The social order or the ‘norm’ is such that people belonging to oppressed caste communities like the Dalits continue to have to carry out tasks involving a high amount of physical labor, the Adivasi communities are forced to reside far away from the cities and Muslims are burdened with financial exploitation, in addition to religion-based persecution and social stigma that have just been getting worse since 2014.
Speaking to the NewsClick, Khadija from Murshidabad said, “It does not matter if we have a stable job or not if we are economically independent; the fear of getting arrested purely due to our religion never stops.” This sense of fear and anxiety that puts entire communities on edge is a manifestation of the mental health implications that structures that fail its populations have.
This constant systemic discrimination and oppression simply because of one’s religious identity has only increased because of COVID-19. When the Tablighi Jumaat incident took place, many media channels called for draconian measures to be taken to punish them. But the difference in the (lack of) condemnation of millions of Hindus who participated in the Kumbh Mela, violating COVID-19 protocols, have not faced the same anger that was shown in that incident.
The mental health wellness industry often operates from a space of neutrality while trying to make a diagnosis and provide intervention. In the process, it fails to recognise the mental stress that comes from the oppression of the marginalised sections by institutionalised structures. It is important that mental health practitioners become more aware and intersectional in their approach, so as to ensure they do not just focus on the classification of a given mental condition and instead, also explore the psychosocial causes behind them.
Most of the therapists around us belong to upper caste groups, making it difficult for a person belonging to an oppressed caste community to reach out and discuss their problems with them. The acknowledgment that well-being and mental health are affected by hierarchical, discriminatory systems such as patriarchy, caste-based and class-based oppression, continues to be missing.
So, when the edifice of this country is built on a system that discriminates against the majority population, you cannot look at an individual’s well-being without factoring in these systemic and structural factors.
Not to mention how other problems interlocked with discrimination against marginalised communities also manifest in accessing therapy. An average therapy session of an hour costs INR 800 or INR 1500. The price itself makes it inaccessible to the majority population. Further, the popular discourse on well-being has become commodified and has become very capitalist in nature.
So, when the edifice of this country is built on a system that discriminates against the majority population, you cannot look at an individual’s well-being without factoring in these systemic and structural factors.
Featured image source: TheWire.in
About the author(s)
Zeba Vagh is pursuing her degree in screen writing from Whistling Woods Mumbai International. An aspiring writer, her work has been published with the Live Wire. She can be found on Instagram.